Hashimoto’s disease is an autoimmune condition that can cause an underactive thyroid, also known as hypothyroidism, or less commonly, an overactive thyroid, known as hyperthyroidism.
Hashimoto’s disease & Chronic thyroiditis
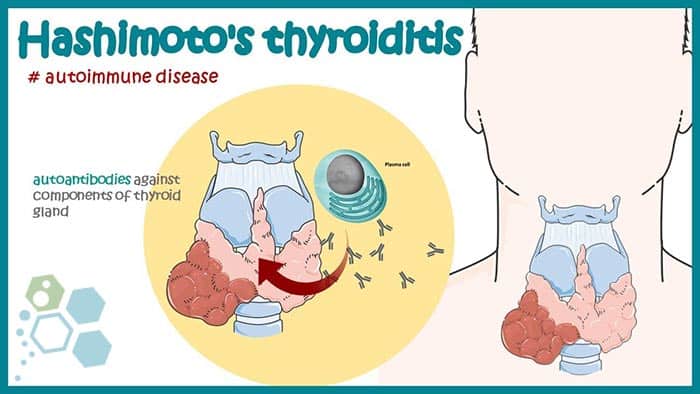
This disease affects the thyroid gland, a small gland in the neck that produces thyroid hormones that control the body’s energy usage and influence various organs, including the heart. Hashimoto’s disease produces antibodies that attack the thyroid gland, accumulating white blood cells in the gland and ultimately leading to its damage, impairing its ability to produce enough thyroid hormones [1].
Hashimoto’s disease is also called:
- Hashimoto’s thyroiditis
- Autoimmune Thyroiditis
- Chronic lymphocytic thyroiditis
Current research shows that Hashimoto’s disease is four to ten times more common in women than men and is likely to develop more often in women aged 30-55. It can also be hereditary, and individuals who have a family history of thyroid diseases or other autoimmune disorders such as Thymoma-associated myasthenia gravis, Type 1 diabetes, Ankylosing Spondylitis, Lupus, Connective Tissue Disease, Rheumatoid Arthritis, autoimmune pancreatitis, and Sjogren’s Syndrome are at a higher risk of developing it. Learn more about genetic testing for Autoimmune diseases.
What does Hashimoto’s disease do to a person?
What are the symptoms of Hashimoto’s disease?
The symptoms of Hashimoto’s disease may not be apparent initially. However, as the condition progresses, the symptoms and complications from hypothyroidism may include:
- Fatigue

- Sudden weight gain
- Constipation
- Apnea (difficulty in breathing)
- Intolerance to cold temperature
- Irregular menstrual periods or fertility problems
- Menorrhagia (abnormally heavy bleeding during menstruation)
- Loss of libido resulting in ED
- Joint and muscle pain associated with osteoporosis & osteoarthritis
- Macroglossia (enlarged tongue)
- Liver inflammation, fibrosis, and necrosis
- Loss of memory and brain fog
- Blockage of the Airway resulting in COPD and Lung Fibrosis
- Ataxia (difficulty in coordination, balance, and speech)
- Depression
- Type 2 Diabetes
- Peripheral neuropathy
- Renal Disease & glomerulonephritis
- Hair thinning or dryness
- Bradycardia (Slowed heart rate)
What tests are used to confirm Hashimoto’s disease?
Treatments for Hashimoto’s Thyroiditis
Once Hashimoto’s disease is diagnosed, treatment often involves thyroid hormone replacement therapy, such as synthetic T3, T4, or desiccated thyroid extract. Hormone replacement therapy involves taking a pill containing synthetic thyroid hormone, which helps replace the hormones your thyroid can no longer produce. Your doctor will monitor your hormone levels and adjust your medication to keep your levels within a healthy range. Some endocrinologists may also prescribe patients a synthetic version of T3 & synthetic T4 for treating Hashimoto’s. This combination is sometimes used for patients who have persistent chronic hypothyroid symptoms but have normal TSH levels. In addition to medications, some lifestyle changes can help manage Hashimoto’s disease. A healthy, balanced diet rich in nutrients, particularly iodine and selenium, can help support thyroid function [3].
Regular exercise can also help manage symptoms, boost energy levels, and improve mood. Working closely with your doctor to manage Hashimoto’s disease is essential, as untreated hypothyroidism can lead to serious health complications. However, most people with non-complicated Hashimoto’s disease can live healthy, fulfilling lives with proper treatment and management.
TREATMENT RISKS & PRECAUTIONS
Please note that not all patients are good candidates for treating Hashimoto’s Disease or Chronic Thyroiditis with stem cells. Patients with severe complications, such as advanced thyroid dysfunction, significant cardiovascular issues, or other coexisting autoimmune disorders, may not be good candidates for treatment.Stem Cell Treatment for Hashimoto’s Disease
Isolated and Expanded UC-MSC+ cells have unique properties, such as being easily harvested from various stroma (autologous and allogeneic), carrying Major Histocompatibility Complex (MHC) antigens that are not frequently expressed, and being able to target injured organs or tissues. These properties make them promising for treating immune diseases, especially autoimmune disorders like Hashimoto’s.
New treatment for Hashimoto’s thyroiditis
Stem Cell Therapy for Thyroid Issues
Role of stem cells in thyroid cell differentiation, thyroiditis & thyroid cancers
Stem cells are categorized based on their origins, including embryonic-derived stem cells (ESCs), mesenchymal stem cells (UC-MSCs), peripheral blood stem cells, organ resident stem cells (RSCs), cancer stem cells (CSCs), perinatal stem cells, and induced pluripotent stem cells (iPSs). The isolated and expanded UC-MSC+ stem cells The Regeneration Center uses originate from the stroma surrounding organs and other tissues such as the umbilical cord and placental tissue [5]. Some organs, such as the brain, liver, and thyroid, have their stem cells. Stem cells are also categorized based on their differentiation potency, ranging from totipotent, multipotent & unipotent cells that can be used in stem cell treatment for inclusion body myositis.The potential applications of stem cells in regenerative medicine have been widely studied and have shown the capacity to develop into organs or tissues such as livers, hearts, skeletal muscles, and kidneys, as well as aid in the development of the nervous system for patients with neurodegenerative diseases such as ALS, MND, Alzheimer, Parkinson’s disease, brain injuries, multiple sclerosis, strokes, and spinal cord injuries. The challenge with stem cell therapy is imitating the complex microenvironments required for organ differentiation. Generated organs or tissues from stem cells without the proper types of cytokines, proteins, and growth factors will lead to poor results. The transplanted cells will lack the necessarily affiliated cells and cannot function as natural ones.
Stem cell treatment for rheumatoid arthritis represents a promising new treatment option that will revolutionize the management of this chronic and debilitating disease. Although the biological treatment is still in the early stages of stem cell science, the results are encouraging, and we will only continue to get better results over time.
Cost of Treating Hashimoto’s with Stem Cells
UC-MSC+ Stem Cell treatment for Hashimoto’s & Chronic Thyroiditis will require an estimated 10-14 days in total. Due to the varying degrees of severity, our medical team will need to evaluate the current health of all potential patients to recommend an appropriate protocol. Upon completion of the medical review, a detailed treatment plan will be provided, including the types and quantities of cells, the total number of nights required, and the total medical-related costs for the entire program. To begin the evaluation process for our multi-stage rheumatoid arthritis treatment using stem cells, please prepare your recent medical records such as radiology scans w/ blood test results and contact us today.
Published Clinical Citations
[1] ^Tempark T, Deekajorndech T, Chatproedprai S, Supornsilchai V, Wananukul S. Late sequelae of drug reaction with eosinophilia and systemic symptoms (DRESS) cause thyroid dysfunction and thyroiditis in Thailand: review of literature. J Pediatr Endocrinol Metab. 2022 Feb 4;35(5):567-575. doi: 10.1515/jpem-2021-0685. PMID: 35119800.
[2] ^ Rajatanavin R. Postpartum thyroid dysfunction: a viewpoint from Thailand. Ann Acad Med Singap. 1993 Jul;22(4):587-92. PMID: 8257065.
[3] ^Coppola A, Tomasello L, Pitrone M, Cillino S, Richiusa P, Pizzolanti G, Giordano C. Human limbal fibroblast-like stem cells induce immune-tolerance in autoreactive T lymphocytes from female patients with Hashimoto’s thyroiditis. Stem Cell Res Ther. 2017 Jul 3;8(1):154. doi: 10.1186/s13287-017-0611-5. PMID: 28673339; PMCID: PMC5496215.
[4] ^Al-Suhaimi EA, Al-Khater K. Functions of stem cells of thyroid glands in health and disease. Rev Endocr Metab Disord. 2019 Jun;20(2):187-195. doi: 10.1007/s11154-019-09496-x. PMID: 31025266.
[5] ^ Giolito MV, Plateroti M. Thyroid hormone signaling in the intestinal stem cells and their niche. Cell Mol Life Sci. 2022 Aug 10;79(9):476. doi: 10.1007/s00018-022-04503-y. PMID: 35947210.

