The word “In vitro” Latin translation, is simply “in glass.” In modern times this means an in-vitro environment is simply in a test tube or laboratory dish that holds the cell culture medium or substance necessary to perform a culture test or fertilization.[1] In vitro fertilization (IVF) is a medical procedure in which eggs and sperm are combined outside the body to create embryos. These embryos are then implanted in the uterus in hopes of achieving a successful pregnancy. IVF is a common treatment for various forms of infertility.
How IVF Works
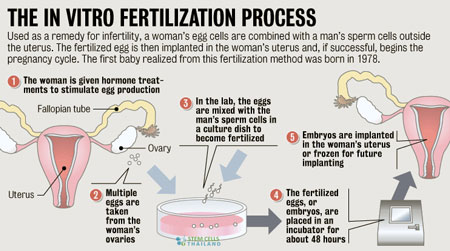
Step-by-step overview of the IVF process:
- Ovarian Stimulation: The woman is given fertility drugs to stimulate the ovaries to produce multiple eggs. Regular ultrasounds and blood tests monitor the development of the follicles (small fluid-filled sacs in the ovaries that contain the eggs).
- Egg Retrieval (Oocyte Retrieval): Once the follicles reach a certain size, indicating maturity of the eggs, the eggs are retrieved from the ovaries. This is typically done via a minor surgical procedure using ultrasound guidance. A thin needle is passed through the vaginal wall to the ovaries, and the eggs are aspirated.
- Sperm Collection: On the day of egg retrieval, a sperm sample is collected from the male partner (or a sperm donor). The sperm is then processed and prepared for fertilization.
- Fertilization: The eggs and sperm are combined in a laboratory dish to allow fertilization to occur. In some cases, especially when there are concerns about sperm quality, a single sperm may be directly injected into an egg using a procedure called intracytoplasmic sperm injection (ICSI).
- Embryo Culture: After fertilization, the embryos are cultured in the laboratory for several days. Their development is monitored, and the best-quality embryos are selected for transfer.
- Embryo Transfer: One or more embryos are selected for transfer into the woman’s uterus. This is a relatively simple procedure that usually doesn’t require anesthesia. A thin catheter is used to place the embryos in the uterus.
After the transfer, the woman is usually given medications like progesterone to support the uterine lining and enhance the chances of embryo implantation. About 10-14 days after the embryo transfer, a blood test is performed to determine if implantation has occurred and the woman is pregnant.
Additional points to consider:
- Freezing and Storage: Not all embryos are transferred immediately. Excess good-quality embryos can be frozen (cryopreserved) for future use.
- Risks: While IVF is generally safe, it carries risks like multiple pregnancies (if more than one embryo implants), ovarian hyperstimulation syndrome (a reaction to fertility drugs), and potential complications from egg retrieval.
- Success Rates: The success of IVF varies and can depend on factors like age, cause of infertility, and specific clinic protocols. Generally, younger women have higher success rates.
- Ethical and Emotional Considerations: IVF can raise ethical questions, especially concerning the disposal of unused embryos. It can also be emotionally taxing, as not all cycles result in a successful pregnancy.
Over the years, IVF and related technologies have evolved and improved, providing hope and a solution for many couples struggling with infertility.
In vitro fertilization or IVF pertains to the artificial method of uniting the sperm with the egg. [2] In-Vitro or IVF treatments are usually performed in closed system laboratory environment by Stochastic Differentiation and directed self differentiation instead of the “traditional” and natural process that occurs in a human female body.
IVF treatments are typically used by families who are having difficulties conceiving. IVF is also a way to clone embryonic stem cells and in genetic Pre-Implementation Diagnosis testing or PGD testing for short. PGD when combined with IVF genetic screening can allow us to screen over 130 know genetic deficiencies and diseases as early as 8 days after artificial conceptions.[3]
Published Clinical Citations
[1] ^ Fauser, Bart C J M, and Gamal I Serour. 2013. Introduction: optimal in vitro fertilization in 2020: the global perspective. Fertility and sterility, no. 2. doi:10.1016/j.fertnstert.2013.06.029. https://www.ncbi.nlm.nih.gov/pubmed/23905706
[2] ^ Iyoke, C A, G O Ugwu, F O Ezugwu, L O Ajah, and S G Mba. The role of ultrasonography in in-vitro fertilization and embryo transfer (IVF-ET). Nigerian journal of medicine : journal of the National Association of Resident Doctors of Nigeria, no. 3. https://www.ncbi.nlm.nih.gov/pubmed/24180141
[3] ^ Jin, Hai-Xia, Zhi-Min Xin, Wen-Yan Song, Shan-Jun Dai, and Ying-Pu Sun. Effects of human cumulus cells on in vitro fertilization outcomes and its significance in short-term insemination. The Journal of reproductive medicine, no. 1-2. https://www.ncbi.nlm.nih.gov/pubmed/23447919