A new study about the long-term effects of COVID has shown a substantial rise in the risk of developing cardiovascular disease, including heart attack and brain strokes, after a SARS-CoV-2 infection. These findings show that even fully vaccinated patients with very mild cases of COVID-19 from omicron subvariant can increase the risk of cardiovascular and pulmonary disease for at least a year after the initial diagnosis. Based on the new data, it appears that the rates of many medical conditions, such as COPD, heart disease and kidney failure, were substantially higher in people who have recovered from exposure to COVID-19 than in similar patients who were never diagnosed with COVID-19. The Regeneration Center did publish our early finding about how covid can lead to heart and lung disease nearly two years ago and the new research seems to confirm our findings.
Additional data found that the risk of developing chronic diseases was seriously high even for patients under 65 years old who lack other risk factors, such as diabetes, liver disease or obesity. The study shows that it doesn’t matter if patients are old or young; it doesn’t matter if they smoked cigarettes or didn’t. The additional risk is there regardless. The researcher compared more than 175,000 people who survived for at least one month (30 days) after contracting COVID-19. The study subjects were divided into two groups of uninfected patients: more than seven million people who used insurance during the pandemic and a similarly sized group that used the insurance before SARS-CoV-2 infection began.
Troubled weak hearts after COVID
Patients who recently recovered from COVID-19 have shown rapid increases in over 21 cardiovascular conditions for over one year after the infection. For example, patients were 53% more likely to have had a brain stroke than the control group, which means that, out of every 1,000 people who participated, there were around five more people in the COVID-19 (exposed) group than in the control group (non-exposed) who experienced having a stroke.
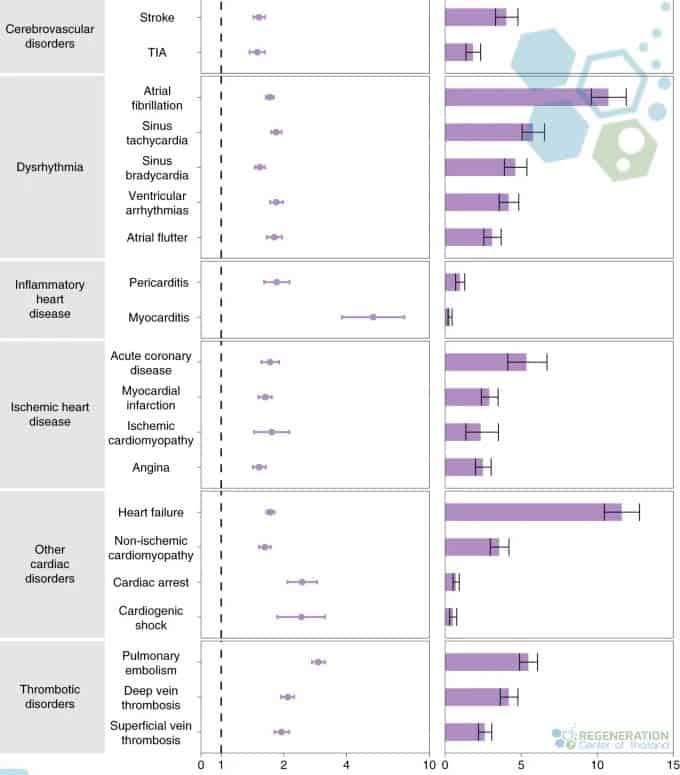
The risk of developing congestive heart failure increased by 70%, or around 11 more people in the COVID-19 group per 1,000 studied. Hospitalization rates also increased other risks, such as the likelihood of developing cardiovascular complications in the future, but even patients who avoided being hospitalized were still at a higher risk for many medical conditions such as dilated cardiomyopathy, transverse myelitis, neuropathy and SLE.
The research reveals how long cardiovascular complications caused by COVID can last. Because severe disease increases the risk of complications far more than a mild case, individuals who are not yet vaccinated must receive their vaccines as soon as possible. The study’s length and observational design impose some limitations. For example, people in the primary control group were not all tested for COVID-19, so it is quite possible that some of the subjects had mild infections which went unreported or un-diagnosed. As the pandemic nears the end, healthcare providers and regenerative healthcare centers worldwide should prepare to address the massive increases in onset cardiovascular disease. But with high COVID-19 case counts that are still straining medical resources around the world, international health authorities might delay preparing for the pandemic’s aftermath for much too long, especially for the millions of patients with long COVID.