Spinal Stenosis is a medical condition characterized by the narrowing of the spinal canal, resulting in increased pressure on the spinal cord and nerve roots. This condition can be congenital or developed over time due to age-related changes in the spine, such as bone spurs and thickened ligaments. It can cause pain, numbness, and weakness in various body parts, depending on where it occurred.
The most common symptoms associated with spinal Stenosis include pain and numbness along the back or legs that worsens with standing or walking and is relieved after sitting down or leaning 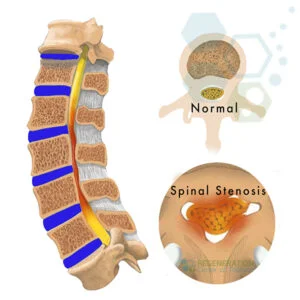
Potential causes of spinal Stenosis can include other age-related changes like herniated discs, arthritis formation within joints, thickening of ligaments, a buildup of bony growths (bone spurs) that pinch nearby nerves, trauma such as an injury causing misalignment in vertebrae which can decrease available space or diseases like Paget’s disease which involve excessive bone growth. Additionally, tumors and cysts may contribute to reduced areas for nerve pathways within the spine.
Symptoms of spinal stenosis can vary depending on the severity of the condition and where it is located. Some common symptoms include pain in the lower back, buttocks or thighs; cramping in the legs or arms; weakness or numbness in the legs, arms, hands or feet; tingling sensation in the back or extremities; difficulty walking for long distances; balance issues such as feeling unsteady when turning or bending.
Potential causes of Spinal Stenosis can include bulging discs, bone spurs (osteophytes) developing on either vertebral facet joints, hypertrophy of surrounding ligaments like the supraspinous ligament and intraspinal enlargements from tumors or nerve entrapment. In addition to these causes specifically causing spinal stenosis, other conditions like osteoarthritis and lumbar spondylolisthesis have been linked with stenosis development through their mechanical effects on nerves [2].
When the spinal column narrows it may press on the spine, compressing the root nerves resulting in pain. Causes for a diagnosis can vary greatly, ranging from genetics to activity level to age-related wear and tear. Other potential risk factors for spinal Stenosis include previous injuries (especially from a fall), ankylosing spondylitis, metabolic diseases, diminishing bone density as we age (osteoporosis), scoliosis, arthritis, tumours, and viral or bacterial infections such as lyme disease. A history of being born with a congenitally narrow spinal canal is also associated with a higher risk of developing the condition later in life.
Diagnosis of spinal stenosis in the cervical (neck area) or lumbar (lower back) can be made through various means, including physical examination, imaging tests (CT scan and MRI scan), myelogram, electrical studies (nerve conduction tests), and musculoskeletal tests. Your orthopedic doctor may check the limbs for reflexes and strength during the initial physical examination. Patients are tested performing simple neurological tasks. Imaging scans are also used to identify bone structure compression or narrowing. Types of radiology scans can include: X-rays,MRI scans, CT scans and Ultrasound. MRI scans are especially helpful for cross-sectional images using magnetic fields and radio waves. In some cases, a myelogram may also be ordered, requiring contrast dye to determine if there are any blockages in the area. Non-invasive electrical studies and nerve conduction tests can be used to assess how well nerves respond to stimuli. At the same time, biochemistry tests can check for evidence of infections or inflammation, as secondary infections have been known to cause spinal stenosis.
Depending on the stage and severity, doctors may recommend certain lifestyle modifications, such as physical therapy, to help enhance overall strength and flexibility and reduce inflammation in tissues around your spine. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be prescribed to help reduce pain and swelling for patients with . Steroids could be used if more severe inflammation is found, accompanied by spasms throughout surrounding muscles. In some cases, surgery may be suggested to increase available nerve paths, which will alleviate pressure caused by spinal Stenosis. Surgery may require rods or screws combined with fused vertebrae sections.
Surgical treatment options may include:
For many patients stem cell therapy offers a non-surgical alternative to treat degenerative discs and spinal stenosis has been proven to show improvements in several areas. Depending on patient needs, stem cells from different sources (autologous vs allogenic) have varying degrees of effectiveness in promoting differentiation and to produce desired biological effects. Since 2007 the Regeneration Center has developed a deep understanding of stem cell therapies for low back pain (LBP), Intervertebral disc degeneration (IDD), acute spinal injuries, spinal stenosis and intervertebral disc herniation.
Isolated and expanded stem cells have been used to intervene in the spinal stenosis process, inflammation to help slow down progression, boost stem cell production, and achieve repair through the cell regeneration process. The Regeneration Medical Center currently offers several types of cell therapies including:
The three main functions for regenerative stem cells are:
Types of Stem Cells and Delivery Methods: Isolated and Expanded Mesenchymal Stem Cell (MSC+) protocol for stenosis will depend on the severity of the underlying condition. Our isolated stem cells do not require any invasive surgeries, and our unique multi-vector delivery of the stem cells which can be done via radio guided direct or Intrathecal Injections along with IV Drips. To learn about the basics of stem cells, visit here[5].
Safety and efficacy are as important as results therefore our unique multi-stage cellular therapy for spinal stenosis will require 1-2 Weeks in Bangkok, Thailand. Due to the varying degrees of spinal damage experienced by each patient, our orthopedic team will need to evaluate potential candidates. Upon approval, a detailed treatment plan will be provided an will include specific recommendations such as day by day treatment calendar (appointment dates), th total number nights required along with fixed medical costs (excluding accommodations or flights). To begin the treatment evaluation process please prepare recent medical records such as (MRI or CT Scans) and contact us today.
Post-Treatment Physical Rehabilitation & Pain relief: For patients with Cervical Stenosis with myelopathy, Ankylosing spondylitis (spinal stenosis) or osteoporosis, physical rehabilitation after your treatment f is optional depending on travel limitations. Total post-therapy rehab plans are also available for 2-4 hours per day and up to 5 days per week. We also offer complete regenerative medical packages, assistance with medical visas and extended stay accommodations for the patient + family upon request.
[1] ^Kasai Y, Paholpak P, Wisanuyotin T, Sukitthanakornkul N, Hanarwut P, Chaiyamoon A, Iamsaard S, Mizuno T. Incidence and Skeletal Features of Developmental Cervical and Lumbar Spinal Stenosis.Intermittent Neurogenic Claudication Asian Spine J. 2022 May 10. doi: 10.31616/asj.2022.0015. Epub ahead of print. PMID: 35527532.
[2] ^Lee JY, Whang PG, Lee JY, Phillips FM, Patel AA. Lumbar spinal stenosis. Instr Course Lect. 2013;62:383-96. PMID: 23395043.
[3] ^Chaimongkhol T, Thiamkaew A, Mahakkanukrauh P. The characteristics of osteophyte around lumbar vertebral foramina associated with spinal stenosis. Anat Cell Biol. 2019 Jun;52(2):143-148. doi: 10.5115/acb.2019.52.2.143. Epub 2019 Jun 30. PMID: 31338231; PMCID: PMC6624344.
[4] ^ Vadalà G, Ambrosio L, Russo F, Papalia R, Denaro V. Stem Cells and Intervertebral Disc Regeneration Overview-What They Can and Can’t Do. Int J Spine Surg. 2021 Apr;15(s1):40-53. doi: 10.14444/8054. Epub 2021 Apr 21. PMID: 34376495; PMCID: PMC8092931.
[5] ^ Sivakamasundari V, Lufkin T. Stemming the Degeneration: IVD Stem Cells and Stem Cell Regenerative Therapy for Degenerative Disc Disease. Adv Stem Cells. Halo Vest vs. Spinal Fusion 2013;2013:724547. doi: 10.5171/2013.724547. PMID: 23951558; PMCID: PMC3742038.